Automating Patient Discharge Workflows in Healthcare with AI
Date
Apr 06, 26
Reading Time
12 Minutes
Category
Generative AI
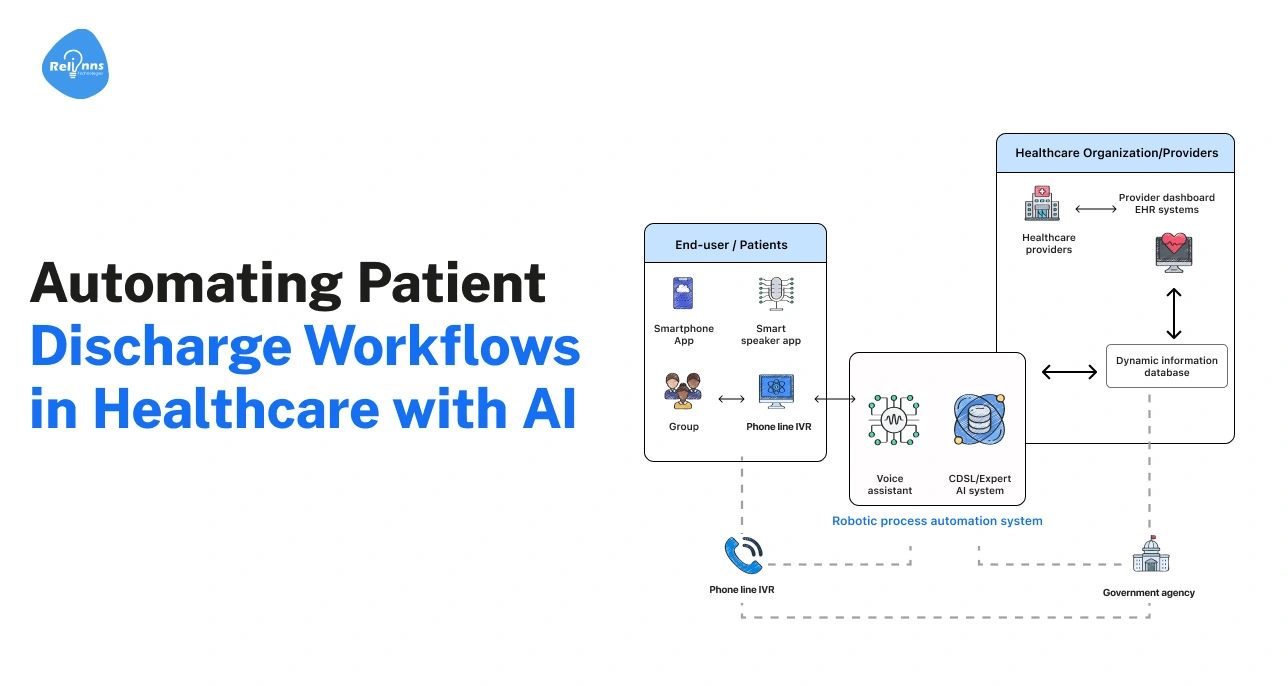
Most hospital beds aren’t blocked by patients; they’re blocked by paperwork.
Discharge delays are one of healthcare’s most expensive and preventable problems. A patient is medically ready to leave, but the summary isn’t written, the pharmacy hasn’t signed off, and no one has confirmed the follow-up.
The result? Beds stay occupied. Costs rise. Patients get frustrated.
Hospitals are now turning to automation and AI to fix this. Automating patient discharge workflows helps care teams move faster, coordinate better, and send patients home safely.
In this guide, you’ll learn how hospitals automate patient discharge workflows, where the process breaks down, and how AI helps fix it.
What Is Patient Discharge Workflow Automation in Healthcare?
Patient discharge automation is the use of technology to streamline and manage the steps involved in patient discharge.
Instead of relying on manual coordination, it automates tasks like documentation, approvals, medication reconciliation, and follow-ups. This reduces delays and ensures nothing is missed.
Today, hospitals are going a step further by using artificial intelligence to make these workflows smarter. AI can predict discharge readiness, generate summaries, and improve coordination across teams.
If you're exploring this shift, you can also read our guide on how AI is enhancing healthcare workflows.
Why Patient Discharge Workflow Automation Matters
Hospitals are increasingly looking for ways to automate patient discharge workflows to reduce delays and improve care transitions.
Here's a look at why getting a discharge right is one of the most important things a hospital can do:
Impact on Patient Outcomes and Readmissions
When discharge steps are manual and inconsistent, important details get missed. Patients leave without clear instructions or follow-ups. This increases the risk of errors and avoidable readmissions.
Automating discharge workflows ensures consistency, accuracy, and timely communication at every step.
For example, a patient discharged without a clear medication schedule is far more likely to miss doses, mismanage their recovery, and end up back in the emergency room within 30 days (a costly outcome for both the patient and the hospital).
Effect on Hospital Efficiency and Bed Turnover
Manual coordination slows everything down.
Patients who are ready to leave stay longer due to pending approvals, documentation, or pharmacy delays. Workflow automation removes these bottlenecks, helping hospitals free up beds faster and improve throughput.
In a busy hospital, a two-hour delay in discharge doesn't just affect one patient. It backs up admissions, clogs the ED, and strains the entire floor.
Role in Care Continuity and Patient Experience
Discharge connects hospital care with recovery. Without structured workflows, this transition feels fragmented.
Automation ensures smoother handoffs, timely updates, and better communication, creating a more reliable and patient-friendly experience.
For patients, leaving a hospital shouldn't feel like falling off a cliff. It should feel like a supported step forward.
Hospitals can speed up and streamline discharges with the right AI. Partnering with healthcare AI experts like Relinns Technologies helps build custom solutions that automate workflows, improve team coordination, and ensure patients leave safely and on time.
Patient Discharge Process in Hospitals: Steps and Automation Opportunities
Patient discharge is a series of coordinated steps that ensure a patient can safely leave the hospital and continue care outside.
Most of these steps are still handled manually in many hospitals, which is where delays and errors begin. Here’s how the process typically unfolds:
| Step | What Happens | Automation Opportunity |
| Readiness Evaluation | The care team confirms the patient is stable and meets clinical criteria. | Flag patients ready for discharge earlier using data signals. |
| Team Alignment and Approvals | Doctors, nurses, and specialists review and sign off. | Automate notifications and approval workflows. |
| Summary and Documentation | A discharge summary is prepared with key details. | Generate summaries and reduce manual writing time. |
| Medication Planning | Prescriptions are finalized and reviewed. | Identify conflicts and speed up pharmacy coordination. |
| Patient Guidance | Instructions are shared with patients and caregivers. | Deliver clear, personalized instructions automatically. |
| Follow-up Planning | Appointments or referrals are scheduled. | Auto-schedule and send reminders. |
| Final Clearance and Exit | All steps are completed before discharge. | Track status and flag pending tasks in real time. |
This multi-step, multi-team process is exactly why hospitals are now investing in automation and AI to streamline discharge workflows.
Key Challenges in Hospital Discharge Workflows
Even with defined steps, discharge often breaks down in execution. Small gaps across teams and tasks create delays that affect the entire system.
- Gaps in Communication Across Teams: Multiple departments are involved, but updates don’t always flow smoothly. Missed handoffs and unclear responsibilities slow progress.
- Slow Documentation and Summary Creation: Discharge notes are often prepared late. This holds up the entire process, even when the patient is ready to leave.
- Medication Coordination Issues: Prescription reviews and pharmacy approvals can take time, especially when there are conflicts or last-minute changes.
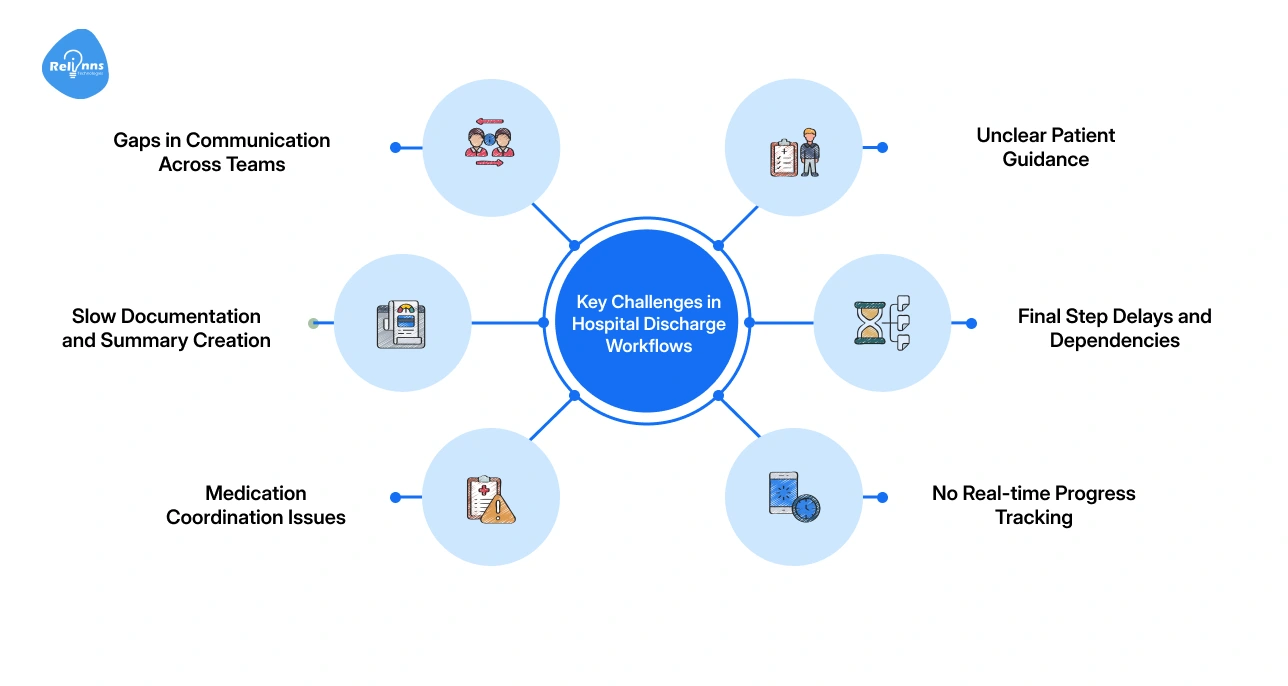
- Unclear Patient Guidance: If instructions are rushed or incomplete, patients may not follow them correctly, increasing the risk of complications.
- Final Step Delays and Dependencies: Transport, pending sign-offs, or small administrative tasks can unexpectedly hold everything up.
- No Real-time Progress Tracking: Teams often lack visibility into what’s completed and what’s pending, making it harder to act quickly.
These challenges aren't isolated; they're systemic. And they compound. One delay triggers another, until a process that should take two hours stretches into six.
This is exactly why manual coordination alone can no longer keep up. Hospitals need smarter systems. Ones that can track, flag, and act in real time. That’s where AI and automation come in.
How Automating Patient Discharge Workflows Improves Outcomes
Automation doesn't just speed things up; it removes the friction that causes delays, errors, and poor patient experiences in the first place.
Here's what changes for discharge workflows in hospitals with automation:
Faster Discharges with Fewer Hold-ups
Routine steps like approvals, summaries, and clearances move without constant follow-ups. This cuts waiting time and helps patients leave on schedule.
For instance, automated task routing ensures that once a physician marks a patient ready for discharge, the nurse, pharmacist, and case manager are notified instantly - no phone calls, no chasing.
Fewer Complications and Return Visits
Clear instructions, accurate records, and timely follow-ups reduce mistakes. Patients are less likely to face issues that lead to unplanned hospital visits.
This includes automated medication reminders, follow-up appointment confirmations, and post-discharge check-in messages that keep patients on track during recovery.
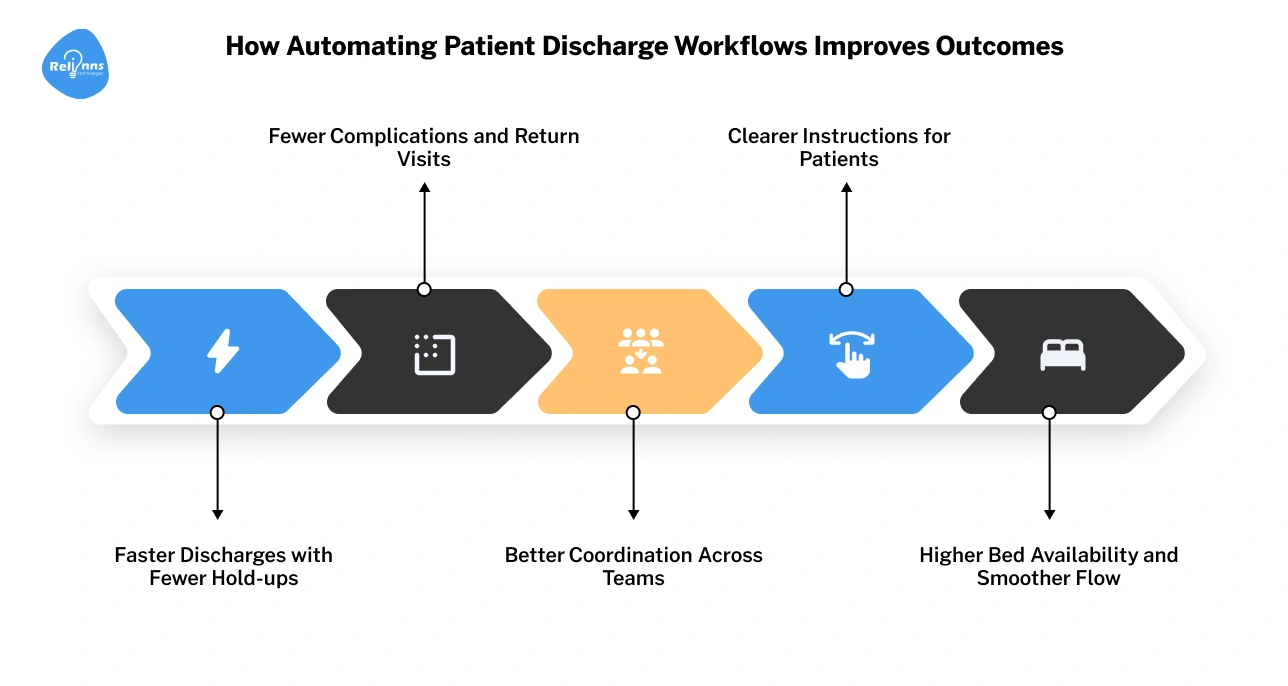
Better Coordination Across Teams
Doctors, nurses, pharmacists, and admin teams stay aligned through shared workflows. Everyone knows what’s done and what’s pending, which streamlines patient discharge.
Tools like Epic and Cerner help healthcare teams centralize discharge tasks, track approvals, and maintain a single source of truth across departments.
Clearer Instructions for Patients
Patients receive simple, structured guidance about medications, recovery, and next steps. This improves how well they follow care plans at home.
Consider: AI-generated discharge summaries that translate complex clinical language into plain, easy-to-understand instructions available in the patient's preferred language and delivered digitally before they leave the building.
Higher Bed Availability and Smoother Flow
When patients leave on time, beds open up sooner. This helps hospitals manage admissions better and maintain a steady flow across departments.
Especially in emergency situations or high-demand periods like flu season or pandemic-like surges, faster discharge cycles can be the difference between a hospital that copes and one that’s overwhelmed.
At this stage, it’s worth understanding the difference between traditional automation and AI, and why AI takes discharge workflows a step further than rule-based systems ever could.
AI vs Traditional Automation in Patient Discharge Workflows
Many hospitals start with rule-based systems, but these often fall short in complex scenarios. AI adds intelligence, helping teams respond faster and make better decisions.
The table below showcases the key differences between traditional rule-based automation and AI-powered automation in patient discharge workflows, and why the gap between them matters in real clinical settings.
| Aspect | Traditional Automation | AI-Powered Automation |
| Approach | Follows fixed rules and predefined workflows (e.g., auto-sending a discharge checklist when a physician marks a patient ready) | Learns from data and adapts to changing situations (e.g., adjusting discharge steps based on a patient's evolving condition or history) |
| Decision-making | Executes tasks based on set logic | Supports decisions using patterns and context |
| Handling complexity | Struggles with exceptions | Adjusts to variations in patient conditions |
| Discharge readiness | Relies on manual checks | Identifies readiness using real-time data |
| Documentation | Requires manual effort | Generates summaries automatically |
| Risk detection | Limited to predefined triggers | Identifies readmission risks using data patterns |
| Visibility | Basic task tracking | Real-time insights with bottleneck detection |
Key Takeaways
- Traditional automation brings structure but breaks down when complexity or exceptions arise.
- AI goes beyond execution; it learns, predicts, and flags issues before they cause delays.
- Rule-based systems need manual input to handle edge cases; AI adapts in real time.
- The strongest discharge workflows combine both: automation for routine tasks, AI for intelligence.
- All AI and automation implementations must adhere to HIPAA and relevant data privacy regulations to protect sensitive patient information.
How AI Adds Power to Patient Discharge Workflow Automation
AI in patient discharge doesn't just connect tasks; it thinks ahead. It interprets patient data, learns from patterns, and surfaces insights that no checklist or rule-based system ever could.
Instead of reacting late, hospitals can now anticipate and resolve issues earlier.
Predicting Discharge Readiness
AI analyzes patient data to identify when someone is ready to leave, helping teams plan earlier and avoid last-minute delays.
Example: A patient recovering faster than expected is flagged early, allowing teams to prepare for a discharge a day in advance instead of waiting for manual review.
Generating Discharge Summaries
Instead of writing summaries manually, AI uses clinical notes, EHR data, and past records to create structured, accurate documents with key clinical details, saving time and reducing errors.
Tools like AI-powered clinical documentation assistants and EHR-integrated copilots can automate this process.
Creating Patient Instructions and Education
AI delivers clear, personalized instructions based on patient history, improving understanding and recovery at home.
This helps patients follow medication schedules correctly and recognize warning signs early.
For example, AI healthcare chatbots can send patients tailored discharge instructions, answer questions in real time, and provide reminders for medications and follow-ups, ensuring clarity and adherence even after they leave the hospital.
Identifying Readmission Risks
By analyzing past data and current signals, AI highlights patients at higher risk, allowing teams to take preventive action.
Think: Patients with chronic conditions, poor medication adherence, or prior readmissions can be flagged before discharge for extra care planning.
Assisting Medication Reconciliation
AI reviews prescriptions and flags potential conflicts, helping reduce medication-related issues after discharge.
For instance, if a patient is prescribed a new medication that interacts with an existing one, AI catches the conflict instantly, before the prescription reaches the patient's hands.
Tracking Discharge Progress and Bottlenecks
AI provides real-time visibility into workflow status, helping teams spot delays and resolve them quickly.
On the whole, every pending task, delayed approval, or incomplete step becomes visible in real time, giving coordinators the clarity to act fast and keep discharge on track.
AI Use Cases in Patient Discharge Across Teams and Scenarios
No two discharges are identical. Patient conditions vary, teams have different responsibilities, and care pathways don’t follow a single script. AI works across all of it, supporting every team and every scenario with the right information at the right time.
Use Cases Across Care Teams
Every team involved in discharge has different responsibilities and different pain points. Here's how AI addresses each one directly:
| Team | AI’s Impact |
| Physicians and Clinical Teams | Earlier readiness flags, faster risk review, quicker decisions |
| Nurses and Case Managers | Full task visibility, cleaner handoffs, fewer missed steps |
| Pharmacy Teams | Automated prescription checks, instant conflict detection |
| Operations and Admin Teams | Delay detection, workflow analytics, smarter planning |
| Patients and Caregivers | Personalized instructions, timely reminders, guided follow-ups |
Next, we'll look at these use cases in the context of real discharge scenarios, because how AI helps a post-surgical patient looks very different from how it supports a chronic care discharge.
Use Cases Across Discharge Scenarios
Discharge looks different depending on the patient, the condition, and the care pathway. Here's where AI makes the biggest difference.
| Scenario | AI’s Role in Discharge |
| General Discharge Coordination | Aligns teams, tracks progress, cuts routine delays |
| Post-surgical Recovery | Monitors recovery signals, triggers timely follow-ups |
| Chronic Condition Management | Personalizes instructions, tracks adherence and risk |
| High-risk Patient Monitoring | Flags vulnerabilities early, enables proactive intervention |
| Multilingual Communication | Delivers instructions in preferred languages, reducing confusion |
Across every team and every scenario, the common thread is the same: AI removes guesswork, reduces delays, and keeps the right people informed at the right time.
Key Features of an AI-Enabled Patient Discharge Management System
A well-designed discharge system brings together workflows, data, and communication in one place. It reduces delays, enhances accuracy, and gives teams better control - while AI adds intelligence to make the process faster and more proactive.
- Seamless Data Integration: Connects with EHRs and hospital systems to keep patient information updated and accessible across teams in real time
- Automated Documentation: Creates discharge summaries using existing patient data, with AI helping structure accurate and complete clinical details
- Smart Task Management: Assigns tasks, sends alerts, and highlights delays or bottlenecks so teams can act quickly
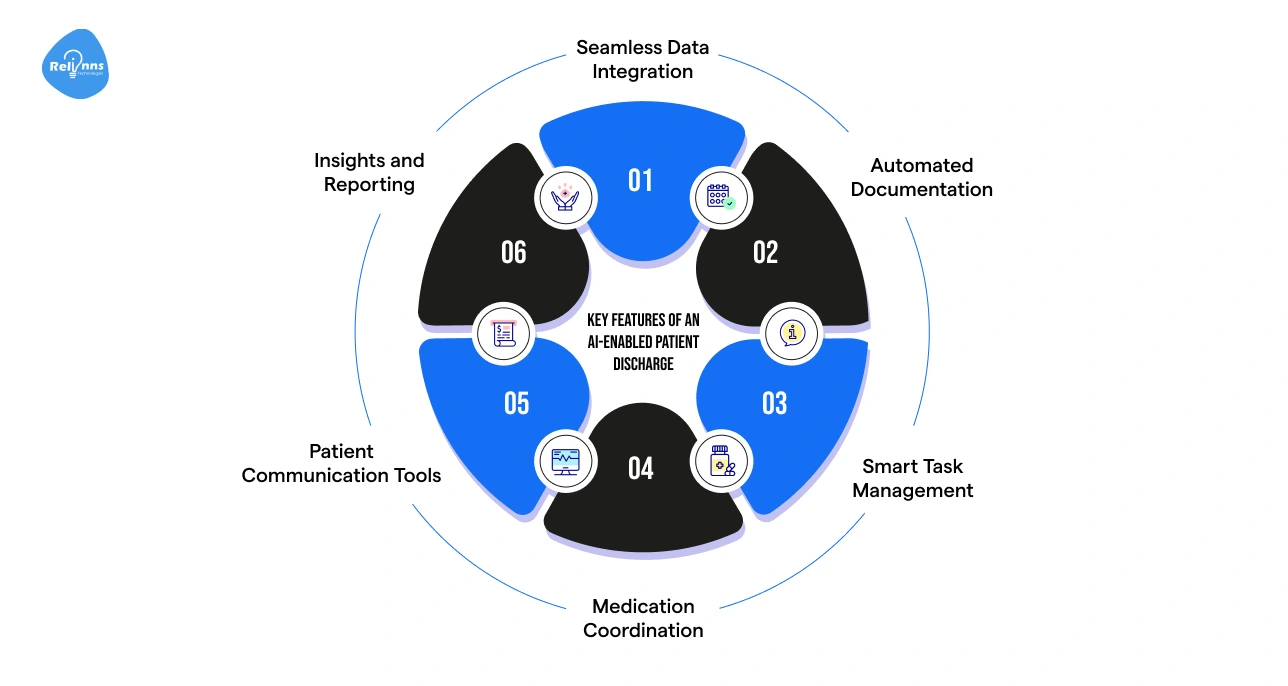
- Medication Coordination: Supports prescription reviews, flags potential conflicts, and ensures accurate medication handling before discharge.
- Patient Communication Tools: Delivers clear instructions, reminders, and follow-ups, with personalization based on patient history and needs.
- Insights and Reporting: Provides dashboards with AI-driven insights to track performance, identify delays, and improve overall workflow efficiency
A strong discharge management system doesn't just digitize paperwork; it actively reduces delays, catches errors before they happen, and keeps every team aligned from the moment discharge is initiated to the moment the patient walks out the door.
How to Build an AI-Powered Patient Discharge Workflow System
Building an effective discharge system starts with structure and evolves with intelligence.
Hospitals need to first fix process gaps, then layer automation, and finally apply AI where it adds real value.
Here's a step-by-step approach to building an AI-powered patient discharge workflow system, one that's practical, scalable, and designed around how hospitals actually operate.
| Step | What to Do | Why It Matters |
| Assess Current Workflows | Map each discharge step and identify delays, handoff gaps, and repeated tasks. | Reveals inefficiencies that slow down the process |
| Set Automation Priorities | Decide which tasks to streamline first based on impact and frequency. | Ensures quick wins and smoother adoption |
| Connect Hospital Systems | Integrate with EHRs and other tools for seamless data flow. | Eliminates data silos and manual updates |
| Apply AI Capabilities | Use AI for predictions, summaries, and risk detection. | Adds intelligence and improves decision-making |
| Maintain Human Oversight | Keep clinical teams involved for validation and final decisions. | Ensures accuracy and builds trust |
| Track and Refine Performance | Monitor key metrics and continuously improve workflows. | Helps optimize efficiency over time |
A Few Things Worth Remembering
While building custom patient discharge workflow automation systems, here are a few key considerations:
- Fix broken processes first. Automation built on a flawed workflow will only make the problems faster.
- Prioritize high-impact areas like documentation and approvals before expanding to complex use cases.
- Integration is non-negotiable. AI is only as good as the data it can access.
- Keep clinical teams in the loop at every stage. Adoption depends on trust, not just technology.
- Treat it as an evolving system, not a one-time implementation; continuous refinement is what drives lasting results.
Essential Metrics for Optimizing Patient Discharge
Tracking the right metrics helps hospitals spot delays, improve coordination, and measure real impact. Focus on a few high-signal indicators that reflect both speed and care quality.
- Discharge Turnaround Time and Delays: This indicates the time from “ready for discharge” to actual exit. (Benchmark: 1-3 hours in efficient systems)
- Readmission Rates and Follow-up Adherence: Tracks patients returning within 30 days and whether follow-ups are completed. (Benchmark: <10-15% readmission; >70-80% follow-up adherence)
- Bed Turnover and Length of Stay: Measures how quickly beds are freed and the average patient stay. (Benchmark: LOS aligned with case mix; faster turnover without compromising care)
- Documentation Completion Time: Time taken to finalize summaries and paperwork. (Benchmark: Within 24 hours; leading systems aim for same-day completion.)
- Staff Productivity and Workload Reduction: Assesses time spent on coordination vs care delivery. (Benchmark: Noticeable reduction in manual tasks and admin time)
When tracked consistently, these metrics give hospitals a clear view of what’s working, what’s slowing things down, and where targeted improvements can drive faster, safer, and more efficient discharges.
Hospitals can turn insights into action with the right technology. Partnering with experts like Relinns Technologies helps build AI-driven discharge solutions that track metrics, automate tasks, and improve patient outcomes.
AI Implementation Challenges in Patient Discharge (and How to Address Them)
AI can transform discharge workflows, but hospitals need to navigate certain challenges to make it effective. Each obstacle has a solution that ensures safe, reliable, and practical implementation.
Here are the main challenges that arise when implementing AI in patient discharge:
Data Quality and EHR Dependency
Challenge: AI relies on accurate, complete data. Inconsistent or outdated EHR entries can lead to incorrect predictions.
For instance, if a patient’s medication history hasn’t been updated after a recent procedure, AI may generate a discharge summary with conflicting prescriptions, creating a risk that's harder to catch than a manual error.
Solution: Regularly audit data, standardize inputs, and integrate AI closely with EHR systems to ensure real-time accuracy.
Clinician Trust and Workflow Adoption
Challenge: Staff may resist AI recommendations if they don’t understand or trust the system. It's critical to bring clinicians into the process early; not as end users of a finished product, but as active participants in shaping how it works.
Solution: Involve clinicians in system design, provide training, and allow human oversight to validate AI decisions.
Accuracy and Validation of AI Outputs
Challenge: AI may produce errors or miss edge cases. Blind reliance can be risky.
Think: A discharge readiness prediction that misses a subtle lab abnormality, or a summary that omits a key diagnosis, can have real consequences for patient safety. AI needs to be checked, not just trusted.
Solution: Implement continuous monitoring, validation against historical outcomes, and feedback loops to refine AI performance.
Data Privacy and Compliance Requirements
Challenge: Handling sensitive patient information carries legal and ethical responsibilities. Especially for healthcare systems in the US, patient data is governed by HIPAA, and any AI implementation that touches protected health information must be built with compliance as a foundation, not an afterthought.
(Read more: HIPAA-Compliant SaaS Checklist and Requirements)
Solution: Encrypt data, apply access controls, and ensure compliance with HIPAA, GDPR, and local regulations.
Avoiding Over-Automation and Workflow Friction
Challenge: Too much automation can overwhelm staff or disrupt established processes. It’s easy to automate for the sake of efficiency and end up creating a system that's faster but harder to use.
Solution: Automate high-value tasks gradually, keep human oversight, and continuously assess workflow impact to maintain balance.
When addressed thoughtfully, these challenges turn AI from a theoretical tool into a practical, reliable partner in patient discharge.
Final Thoughts
Patient discharge doesn’t have to be slow, confusing, or error-prone. Automation and AI make the process faster, safer, and more dependable. They help teams coordinate, reduce delays, and guide patients clearly through next steps.
Hospitals that adopt these technologies and automate patient discharge workflows can improve outcomes, free up beds, and lower readmissions. The key is combining smart tools with human oversight and ensuring compliance with HIPAA and data privacy rules.
When done right, AI-powered discharge workflows transform a stressful, fragmented process into a smooth, predictable experience for both patients and care teams.
Frequently Asked Questions
What is patient discharge workflow automation?
It’s using technology to streamline discharge steps, reduce delays, and improve communication between care teams, often enhanced with AI for smarter decision-making.
How does AI improve patient discharge processes?
AI predicts discharge readiness, generates summaries, flags readmission risks, and helps coordinate tasks, making hospital discharges faster, safer, and more accurate.
Why is HIPAA compliance important in AI discharge systems?
HIPAA ensures patient data privacy. AI discharge systems must encrypt data, control access, and follow regulations to protect sensitive health information.
What are the benefits of automating discharge workflows?
Automation reduces delays, improves coordination, lowers readmissions, enhances patient understanding, and increases bed availability for efficient hospital operations.
Can AI help reduce hospital readmissions?
Yes. AI identifies high-risk patients, flags potential complications, and ensures follow-ups, reducing avoidable readmissions and improving recovery outcomes.
How do hospitals implement AI-powered discharge systems?
Hospitals map workflows, automate routine tasks, integrate with EHRs, apply AI for predictions, and monitor metrics while keeping human oversight.
What teams benefit from AI in discharge workflows?
Physicians, nurses, case managers, pharmacists, admin teams, and patients all benefit through better coordination, task visibility, and personalized instructions.





