Medical Billing Automation: How AI Is Transforming Billing Systems
Date
Mar 30, 26
Reading Time
10 Minutes
Category
Generative AI
Billing errors quietly drain healthcare revenue.
Most providers don’t realize how much they lose until claims start getting denied, delayed, or underpaid. Teams chase corrections, resubmit claims, and still deal with repeat errors. The process feels stuck, slow, and expensive.
That's where AI-driven medical billing automation comes in. It helps teams catch errors early, reduce denials, and speed up reimbursements. It's not just about saving time anymore. It's about protecting revenue and improving accuracy across the entire billing workflow.
In this guide, we’ll break down how medical billing automation with AI works and where it delivers real impact.
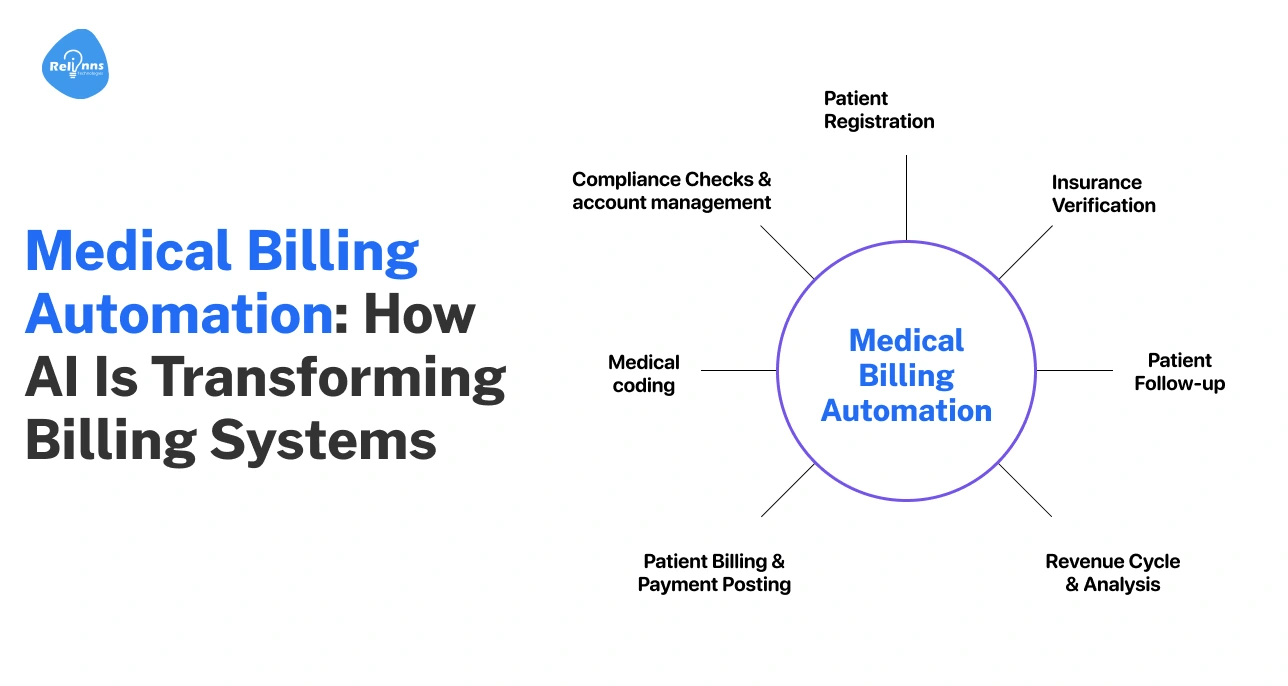
What Is Medical Billing Automation with AI?
Medical billing automation uses software to handle billing tasks like coding, claim checks, and submissions. Instead of manual work, systems follow predefined rules to process claims faster.
Enter artificial intelligence (AI), and this power becomes adaptive. AI doesn't just follow rules; it learns from patterns, catches anomalies, and makes smarter decisions with every claim it processes.
Example: When a claim is submitted with a diagnosis code that rarely pairs with the listed procedure, AI flags it instantly. A rule-based system would let it pass. AI catches it before it ever reaches the payer.
But before we look into the full potential of AI, we'll see how medical billing automation changes the game for healthcare.
Medical Billing Automation vs Manual Processes
Manual billing depends on people reviewing data, assigning codes, and fixing errors. This takes time and often leads to mistakes. On the other hand, automation reduces this effort by handling repetitive tasks, improving speed and consistency.
| Aspect | Manual Billing | Medical Billing Automation |
| Speed | Slow and time-consuming | Fast and efficient |
| Accuracy | Prone to errors | More accurate and consistent |
| Effort | High manual work | Minimal human effort |
| Scalability | Hard to scale | Easy to scale |
This shows why healthcare billing automation is no longer optional for modern operations. Now, we'll look at how AI makes these systems even more powerful.
How AI Enhances Billing Automation Systems
AI takes automation a step further. It can analyze past data, learn patterns, and make smarter decisions. It helps detect errors early, improve coding precision, and reduce claim denials.
For instance, an AI-powered billing system can use natural language processing (NLP) to read clinical notes and automatically suggest the most accurate medical codes, cutting down coder workload while improving precision.
Automation vs AI in Medical Billing
Automation follows fixed rules. It handles repetitive tasks like claim submission and data entry. It works well, but only within what it’s programmed to do.
AI goes further. It learns from past claims, adapts to patterns, and improves over time. It doesn’t just process tasks. It helps prevent errors and predict outcomes.
| Aspect | Automation | AI in Medical Billing |
| Logic | Fixed rules | Learns from data |
| Error Handling | Fixes known issues | Detects hidden patterns and risks |
| Denials | Reacts after denial | Predicts and prevents denials |
| Improvement | No self-improvement | Improves with more data |
AI shifts billing from reactive work to proactive decision-making.
By supporting key steps like coding, claim validation, and denial prediction, it works alongside automation to improve the entire billing process, from submission to payment.
To streamline revenue cycles, many healthcare organizations leverage partnerships with technology experts like Relinns Technologies to build AI-driven billing tools that improve claim processing and prevent denials.
How Medical Billing Works: From Patient Intake to Final Payment
Before understanding where AI fits, it helps to see how medical billing actually works.
The process isn’t a single task. It’s a chain of steps, and a weak link anywhere in that chain can delay payments or trigger denials. Here’s how the workflow typically unfolds:
- Patient Registration and Insurance Capture: Collect patient details, insurance information, and verify basic data accuracy at the first touchpoint.
- Eligibility Verification and Benefits Check: Confirm insurance coverage, policy limits, co-pays, and service eligibility before treatment.
- Medical Coding and Charge Capture: Convert clinical notes into standardized codes and capture all billable services correctly.
- Claim Scrubbing and Submission: Check claims for errors, missing data, or mismatches, then submit them to insurers.
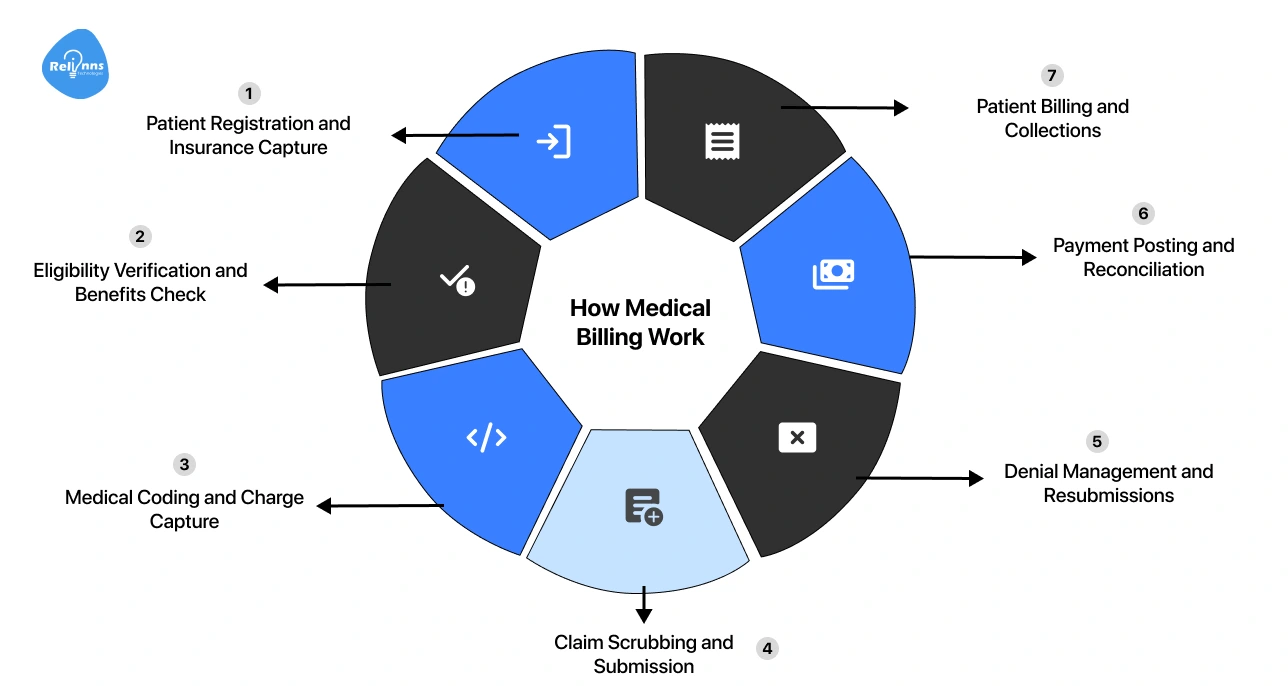
- Denial Management and Resubmissions: Identify denied claims, fix issues, and resubmit them for approval.
- Payment Posting and Reconciliation: Record payments from insurers and patients, and match them against submitted claims.
- Patient Billing and Collections: Generate bills for patients, manage follow-ups, and collect outstanding payments.
Each of these steps carries risk. Manual handling at any point opens the door to errors, delays, and revenue loss. That's exactly where AI-powered automation makes its biggest impact, and we'll cover that next.
How AI Is Transforming Medical Billing Automation and Driving Business Outcomes
AI doesn't just speed up billing. It makes the entire system smarter.
From coding to collections, here's how AI is driving real, measurable outcomes across every stage of the billing workflow.
Medical Coding and Documentation Support
AI in medical coding and billing reviews clinical notes and suggests accurate codes based on context. This reduces manual effort and improves coding consistency. Tools like 3M M*Modal or Nuance DAX assist in clinical documentation and coding accuracy.
For example, it can flag missing documentation like an unsupported diagnosis code, incomplete procedure notes, or a missing provider signature before a claim is created, stopping errors at the source.
Claim Validation and Real-time Error Detection
AI solutions like Optum’s Intelligent Claims Management can check claims before submission and catch errors like missing fields or incorrect codes.
Instead of fixing rejections later, teams prevent them upfront, increasing clean claim rates.
Denial Prediction and Prevention
AI analyzes past claim data to identify patterns that lead to denials. It flags high-risk claims early, so teams can fix issues before submission.
Consider: A hospital submits hundreds of cardiology claims monthly. AI detects that a specific code combination has a 70% denial rate with a particular payer and automatically reroutes those claims for review before they go out.
Revenue Leakage and Undercoding Detection
AI identifies missed charges or under-coded services. For example, it can detect when procedures are billed at lower complexity than documented, helping recover lost revenue.
This helps providers capture every dollar they've rightfully earned, without adding extra review burden on billing teams.
Fraud Detection and Anomaly Identification
AI spots unusual billing patterns that may indicate fraud or errors. This helps reduce compliance risks and supports audit readiness.
Cotiviti's Clinical Fraud, Waste, and Abuse solution helps payers and providers detect anomalous claim patterns (such as duplicate billing or upcoding trends), before they escalate into compliance issues.
Intelligent Patient Billing Communication
AI enables automated, personalized billing messages. Patients receive clear explanations, reminders, and payment options, improving collections and experience.
The impact compounds quickly. Fewer denials, faster reimbursements, recovered revenue, and lower operational costs. AI doesn't just improve billing; it transforms it into a competitive advantage.
Common Challenges in Medical Billing and How AI Addresses Them
Medical billing breaks down when processes get complex, disconnected, and repetitive. Manual effort and rule-based systems can’t keep up.
AI healthcare billing helps fix these gaps by learning from data and acting early. The table below maps the most common billing challenges to how AI directly addresses them.
| Challenge | How AI Solves It |
| Complex Workflows Across Coding, Claims, and Payments | Connects steps and automates decisions across the billing cycle |
| Coding Errors and Incomplete Documentation | Reads clinical notes and suggests accurate codes with context |
| High Denial Rates and Repeated Rework | Identifies patterns behind denials and flags risky claims before submission |
| Slow Reimbursements & Delayed payments | Speeds up claim processing and reduces back-and-forth with insurers |
| Revenue Leakage from Missed or Under-coded Charges | Detects gaps in billing and ensures all services are captured correctly |
| Disconnected Systems and Data Silos | Integrates with EHRs and billing tools to create a unified data flow |
AI shifts billing from reactive fixes to proactive control. Instead of chasing errors, teams prevent them early and keep the revenue cycle moving smoothly.
Key Features of an AI-Powered Automated Medical Billing System
An automated medical billing system combines rule-based workflows with AI to improve accuracy, speed, and control across the billing cycle.
These features reduce manual effort and keep revenue moving without delays.
- Eligibility and Insurance Verification: Checks coverage, benefits, and policy details in real time before claims are created. For instance, if a patient's plan doesn't cover a scheduled procedure, the system flags it at registration.
- Medical Coding and Claim Scrubbing: Suggests accurate codes and flags missing or incorrect data before submission. This helps ensure every service is billed at the right complexity level, protecting revenue from the start.
- Denial Management Workflows: Identifies high-risk claims and helps teams fix issues early to avoid rework. Imagine knowing which claims are likely to get denied before they're even submitted, and resolving them proactively.

- Payment Tracking and Reconciliation: Tracks payments from insurers and patients and matches them with submitted claims. For high-volume practices, this eliminates manual matching errors and ensures no payment goes unrecorded.
- Predictive Analytics and Revenue Insights: Highlights patterns like denials, delays, and revenue gaps to guide decisions. Think of it as a billing dashboard that shows what's likely to go wrong, before it does.
- Integrations with EHR and Billing Systems: Connects with existing tools to ensure smooth data flow across the billing process. For example, a direct integration with EHR systems like Epic or Cerner means clinical data flows into billing automatically, reducing duplicate entry.
With the right features in place, billing teams spend less time fixing errors and more time doing work that actually moves the needle.
How to Implement Medical Billing Automation with AI
Implementing AI in medical billing works best when done step by step. The goal is to start where impact is highest, then expand across the billing workflow without disrupting operations.
| Step | What to Do | Real-world Example |
| Identify High-ROI Areas | Start with processes that cause the most delays or denials. | A hospital targets denial management first after finding a high share of claims are denied due to coding mismatches. |
| Balance Automation with AI | Use rules for simple tasks and AI for complex decisions. | Simple eligibility checks run on rule-based logic while AI handles complex multi-payer claim validations. |
| Integrate with Existing Systems | Connect AI tools with EHR and billing platforms. | A clinic integrates its AI billing tool with Epic, eliminating manual data re-entry between clinical and billing teams. |
| Add Human Review Loops | Keep experts in the loop for validation and edge cases. | AI flags uncertain claims for a senior coder to review before submission. |
| Train Billing Teams | Help teams understand and trust AI outputs. | A billing manager runs weekly sessions explaining how AI flags work and when to override them. |
| Monitor and Improve Continuously | Track performance and refine models over time. | A billing team re-trains its AI model monthly as new payer rules are introduced. |
Key Takeaways
- Start small. Focus on high-impact areas first.
- Combine rules and AI instead of replacing everything at once.
- Keep humans involved for accuracy and trust.
- Integrate deeply with existing systems for smooth workflows.
- Continuously monitor results and improve performance over time.
Measuring What Matters: AI Medical Billing Performance Metrics
Tracking the right numbers shows if AI is actually improving your billing. Here are key metrics to watch, with some benchmark targets that healthcare providers can use as a baseline:
- Claim Acceptance Rates: Percentage of claims approved on the first submission. Aim for 95%+ clean claims.
- Denial Reduction: How many claims are denied compared to before AI? A 30-50% drop is typical.
- Accounts Receivable (AR) Cycle Time: Time from service to payment posting. Look for 20-40% faster cycles with AI.
- Revenue Recovery and Leakage Prevention: Extra dollars captured from missed or under-coded services. Organizations often see 2-5% additional revenue.
- Operational Cost Savings: Reduced hours spent on manual work and rework. Many teams report 25-35% lower administrative costs.
Monitoring these metrics regularly helps ensure AI is delivering real results and keeps your revenue cycle healthy.
For healthcare organizations ready to take the next step, partnering with Relinns Technologies provides custom AI billing solutions tailored to their workflows. From intelligent claim processing to predictive denial prevention, you reduce errors, speed reimbursements, and keep revenue flowing smoothly.
Key Challenges and Risks of AI in Medical Billing Automation
AI in medical billing delivers real results, but only when risks are managed from the start. Here's what to watch for and how to stay ahead of it:
Data Privacy and Security
The Challenge: Billing data is sensitive. AI tools can be a target for breaches. For instance, a misconfigured AI platform with access to patient records could expose thousands of records in a single incident, triggering HIPAA violations and costly penalties.
The Fix: Use encrypted systems, role-based access, and monitor data access. Ensure compliance with HIPAA and other regulations.
Integration with Legacy Systems
The Challenge: Older EHRs or billing software may not sync well with AI solutions. That means data gets stuck in silos, manual workarounds creep back in, and the efficiency gains from AI are quickly offset.
The Fix: Plan phased integration, use APIs, and work with platforms that support modern connectors.
Accuracy and Explainability
The Challenge: AI can suggest codes or detect errors, but mistakes may still happen. Teams may not trust recommendations they don’t understand.
The Fix: Implement human-in-the-loop reviews and choose AI that provides explanations for its decisions.
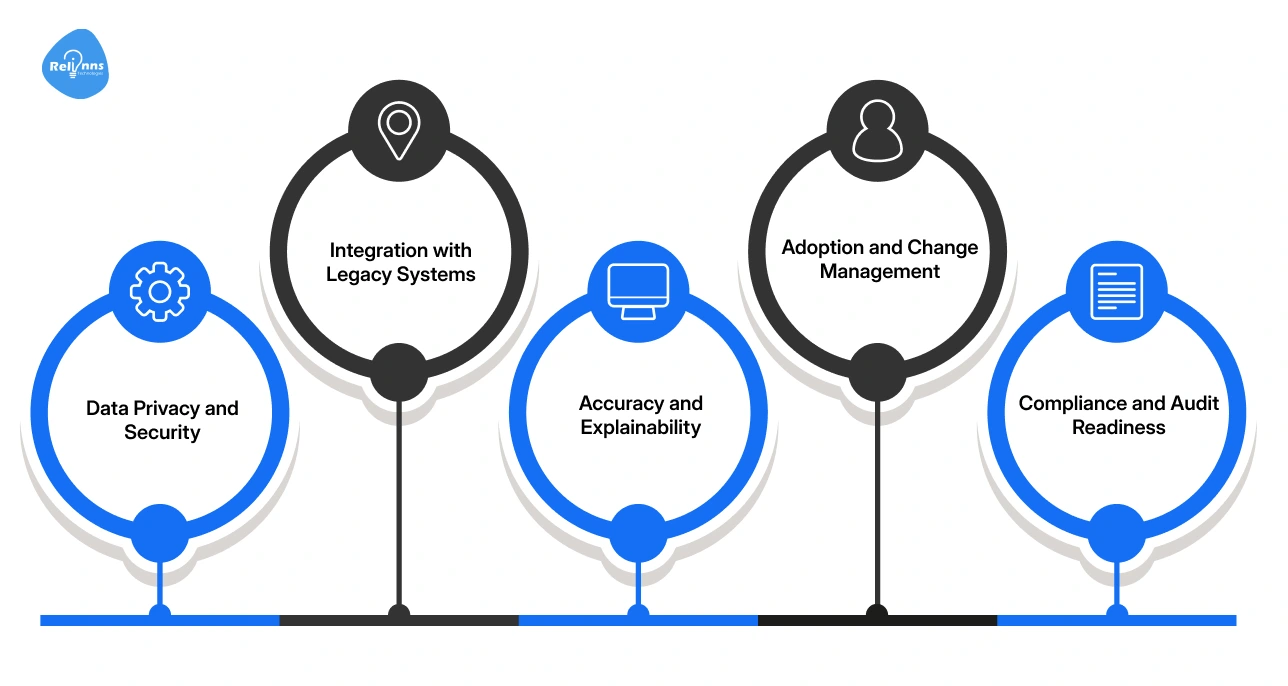
Adoption and Change Management
The Challenge: Staff may resist new tools or struggle to adjust to AI workflows. It's crucial to address this early. Resistance from billing teams can slow down implementation and limit AI's actual impact on the ground.
The Fix: Provide hands-on training, show clear benefits, and involve teams in pilot programs before full rollout.
Compliance and Audit Readiness
The Challenge: AI models can change over time, making audit trails tricky. Especially for US healthcare, HIPAA is non-negotiable, and an AI system that can't explain its decisions creates serious compliance exposure.
The Fix: Keep detailed logs of AI decisions, maintain version control, and regularly review processes for compliance.
AI works best when risks are planned for, not patched later. Get the foundations right, and the benefits follow.
AI Use Cases in Medical Billing Automation for Healthcare
Medical billing automation with AI is being used across different healthcare settings to improve efficiency, reduce errors, and speed up revenue collection.
Here are some key applications to show how different healthcare environments are putting AI to work:
| Healthcare Setting | Use Case | Benefit |
| Hospitals and Health Systems | AI-driven billing for large patient volumes | Reduces claim errors, speeds reimbursements, and improves revenue cycle efficiency |
| Specialty Clinics | AI-powered workflows for niche services | Ensures accurate coding for complex procedures and minimizes denials |
| Multi-location Setups | Scalable AI billing across sites | Standardizes billing practices, centralizes data, and reduces administrative workload |
| Revenue Cycle Management (RCM) Companies | AI-assisted claim processing | Increases clean claim submissions, accelerates payment, and improves client satisfaction |
By implementing AI in these scenarios, healthcare organizations can save time, cut operational costs, and improve accuracy.
The flexibility of AI tools makes them suitable for both high-volume hospitals and specialized clinics, while multi-location and RCM setups benefit from centralized, standardized workflows.
Choosing the Right AI Medical Billing Software: What to Look For
Choosing the right AI medical billing system can save time, reduce mistakes, and keep your revenue flowing.
The trick is to focus on what matters most: intelligence, usability, and fit with your existing processes.
Evaluating AI Capabilities
Look for platforms that don’t just follow rules. Can the system spot potential denials, suggest correct codes, and catch mistakes before they happen?
The smarter it is, the more it can take off your team’s plate.
For example, Waystar's AI-powered claims management tool helps billing teams predict denials, automate claim corrections, and prioritize worklists, reducing manual effort across the entire claims cycle.
Top Features to Look For
The system should simplify key tasks: check patient coverage, review coding, validate claims, manage denials, track payments, and provide actionable insights.
Bonus if it works seamlessly with your existing health records and billing tools.
Questions to Ask Vendors
Before finalizing a platform, it's important to vet every vendor carefully. Here are the questions to ask:
- How reliable is your AI at suggesting codes?
- Can it anticipate and prevent claim issues?
- How does it improve with experience?
- Can we see why it made a recommendation?
- How do you secure patient data and meet regulations?
Integration, Scalability, and Compliance Considerations
Ensure the platform works with your existing EHR, billing software, and multiple sites. Check for HIPAA & GDPR compliance and whether it can scale as your operations grow.
Curious about what makes your SaaS HIPAA-compliant? Learn more in our HIPAA Compliance for SaaS guide.
The right AI billing software doesn't just fit your current needs; it grows with your operations, adapts to new payer rules, and keeps your revenue cycle running without constant manual intervention.
The Future of AI in Medical Billing Automation
Billing is no longer just paperwork. AI is turning it into a smart, proactive process.
The future points to predictive and autonomous systems that catch errors before they happen. Claims will be coded and processed in real time, cutting delays.
Conversational AI will help patients understand bills and pay faster. Entire revenue cycles will run more efficiently, with fewer mistakes and faster cash flow.
Implementing AI today sets the stage for these improvements. The key is to start smart, focus on high-impact areas, and let AI grow with your billing needs.
Frequently Asked Questions
What is AI medical billing automation?
AI medical billing automation uses artificial intelligence to streamline coding, claim processing, and payment tracking, reducing errors and speeding up revenue cycles.
How does AI improve medical billing accuracy?
AI reviews claims, suggests correct codes, detects errors, and predicts denials, ensuring cleaner submissions and fewer claim rejections.
Can AI reduce billing denials?
Yes. AI identifies high-risk claims, highlights missing information, and recommends corrections before submission, lowering denial rates significantly.
Is AI medical billing compliant with HIPAA?
When implemented properly, AI billing systems follow HIPAA and GDPR standards, encrypting data and maintaining secure, auditable workflows.
What features should I look for in AI billing software?
Look for eligibility checks, intelligent coding, claim scrubbing, denial management, payment tracking, predictive analytics, and EHR integrations.
How does AI help healthcare revenue cycles?
AI accelerates claim processing, improves accuracy, predicts denials, and automates repetitive tasks, boosting cash flow and reducing administrative overhead.
Can AI medical billing scale for multi-location practices?
Yes. AI platforms standardize workflows, integrate with multiple systems, and handle high-volume billing across clinics and hospitals efficiently.





